Denver fails to meet emergency response time goals, audit says
A city audit concluded that Denver’s emergency first responders are failing to meet their own response time goals — a situation that managers partly blamed on new laws that resulted in having less control over how often staffers could take a leave of absence.
Emergency managers also said that, as a result, the city needs to hire more 911 operators.
Denver Auditor Timothy M. O’Brien said he sought to evaluate several key aspects of the city’s 911 emergency response system, including alignment with industry standards, adequate staffing levels, oversight and monitoring, the reliability of data used for decision-making, and compliance with contractual obligations.
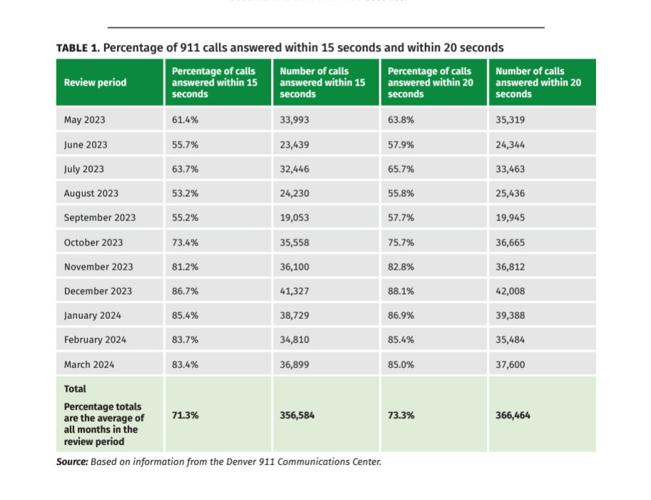
From May 2023 through March 2024, auditors said the Denver 911 Communications Center answered and processed 500,297 emergency calls, averaging 45,000 calls per month — but the center did not meet call answering time goals.
Denver 911 benchmarks its goals using standards set by the National Emergency Number Association to answer 90% of all 911 calls within 15 seconds and 95% of all calls within 20 seconds.
Out of the more 500,000 calls Denver 911 answered, 71% were answered within 15 seconds and 73% were answered within 20 seconds — missing the agency’s 90% and 95% goals, respectively.
“People expect medical emergencies are responded to fast and efficiently,” O’Brien said at a news conference. “Every second matters. Because first responders are falling short of nationally agreed-upon response time goals, they are letting down the people of Denver who need emergency or life-saving medical assistance in critical moments.”
Callers, in some cases, waited for more than a minute for their call to be answered.
Emergency Communication Center Director Andre Dameron agreed with auditors and said staffing shortages have been a significant problem since the pandemic when, at one time, turnover rates were as high as 77%.
Shortages also resulted in 911 operators being required to work up to 14 hours in a 24-hour period and averaging 163 hours of overtime during the 11-month review period.
While the center has made significant strides in hiring and retaining personnel — with turnover rates now at less than 10% — Dameron said recent changes in labor laws also played a role in staffing struggles.
“The Colorado Healthy Workplaces and Families Act, as well as the introduction of the family leave or what the city did with CARE, has meant that we have less control over the amount of leave being taken, and employees have a larger bank to pull from,” he said. “As a result, we’ve seen a 334% increase in the amount of leave being taken by our employees, and that also has had an impact.”
A recent staffing assessment by Denver 911 determined that the agency would need an additional 41 full-time employees to meet the current call volume.
“In order to afford additional FTE, we have to raise the 911 fee for the City and County of Denver,” Dameron said. “That is a process that we are beginning and expect to have completed by this summer, at which point we will have the funds necessary to hire at least 19 additional staff to start.”
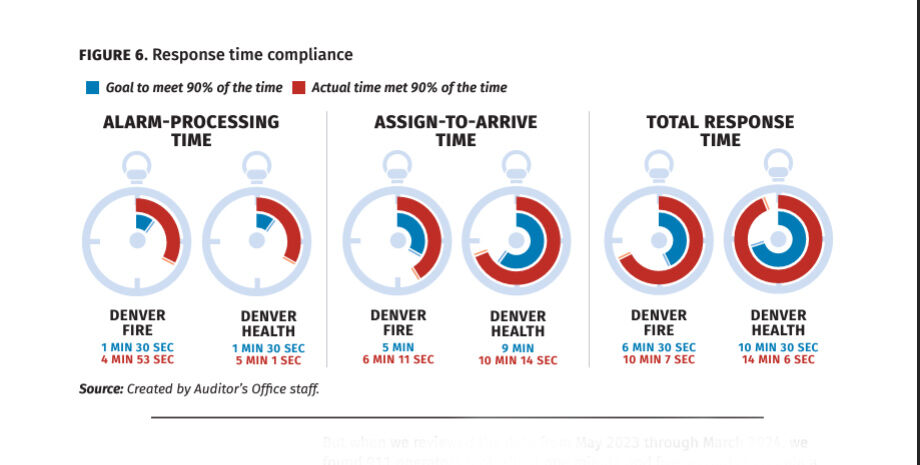
It’s not just the call-answering time that auditors reviewed. They also examined total response time — the time it takes to process, dispatch and travel to an emergency incident.
After analyzing the data for 71,423 Denver Fire Department incidents and 64,868 Denver Health incidents, Auditors found that neither met their response-time goals.
Denver Fire strives to respond to 90% of calls within six minutes and 30 seconds. Auditors found that 90% of calls were responded to within 10 minutes and seven seconds. For Denver Health, 90% of their calls should be met within 10 minutes and 30 seconds. Auditors found that 90% of calls were responded to within 14 minutes and six seconds.
The city’s emergency medical response time goals “are flawed,” the audit noted, and may not take into consideration other factors that could affect performance, such as staffing, population size, inclement weather, traffic congestion and other barriers unique to the metro area.
Denver Chief of Fire Desmond Fulton said similar findings surfaced during the department’s recent accreditation process.
“The one thing that was glaringly apparent from our accreditation, and was brought to our attention, was we have an unrealistic goal,” Fulton told auditors. “Cities our size that have the density that we have, the vertical buildings of 55-plus stories, the warehouses of a million square feet, plus the traffic, the congestion and the construction … it’s just an unrealistic goal.”
Fulton added that as bollards and bike lanes increase, navigating the downtown landscape becomes more challenging.
It’s a case-by-case basis, Fulton said, “especially with construction downtown, the way streets are closed and open changes on a daily basis. We do get notifications, but there are many times where we have to take alternate routes that would absolutely add to the response time overall.”
Auditors also found the city’s method for measuring total emergency medical response times does not align with industry standards or reflect actual 911 caller experiences, recommending that the Department of Public Safety ensure systems used to track emergency medical response should be interoperable and allow data to be collected and reviewed in a central repository.
Agency officials disagreed, noting that data is already being collected by multiple agencies — albeit in different systems with no present system to “coalesce data.”
The Emergency Medical Response System Advisory Committee is responsible for overseeing Denver’s emergency medical response system performance, but it lacks “proper organizational structure,” according to the audit. Suggested improvements included appointing meeting leaders, including an agenda and keeping detailed minutes.
Department of Public Safety Executive Director Armando Saldate agreed with the findings.
“After the pandemic, which affected our department, a lot of meetings were canceled,” he said. “There were remote meetings, and then there was a turnover in staff, also a turnover in staff here in my department. There is turnover in our data analyst that leads the meetings, new council members that we needed to integrate and onboard — all that suffered. We do recognize and agree with all the findings here, and we’ve really worked hard to start that process of creating formalized processes.”
Finally, auditors found deficiencies in the department’s processes for analyzing and validating response time data. Specifically, they noted policies and procedures “lack sufficient detail and appear incomplete.”
Additionally, changes to the data analysis process are not formally reviewed, they said.
The report noted noncompliance issues around the operating agreement the city has with Denver Health.
“We learned that one analyst is assigned the role of maintaining and reporting active response time data and was tasked with independently developing the policies and procedures with little oversight or guidance. The operating agreement states that certain calls must be identified and excluded from the data analysis,” Senior Auditor Maria Durant said.
Saldate disagreed with that finding, arguing that the department documents its processes for data handling but ceded that some adjustments could be made.
“The Emergency Medical Response System — including the Department of Public Safety, Denver 911, Denver Fire Department and Denver Health Paramedic Division — is committed to working collaboratively to get the right resources to the right patients at the right times for all medical emergencies across Denver,” a statement from the Denver Department of Public Safety said. “Led by our dual medical direction team, we are working together to analyze our goals, necessary resources and process improvements for each agency involved in EMRS to find solutions and implement recommendations from the Auditor’s Office to better serve the people of Denver.”